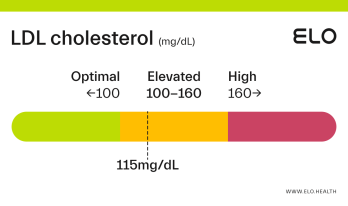
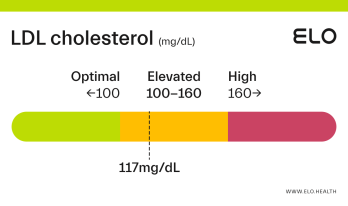
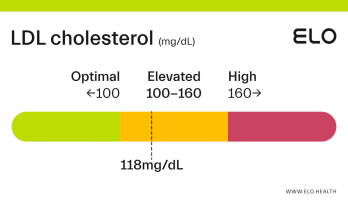
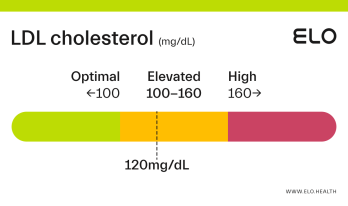
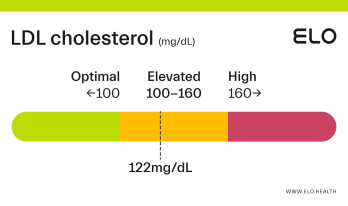
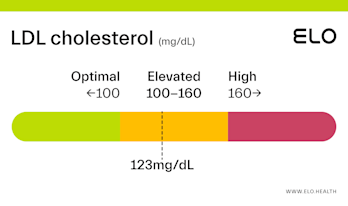
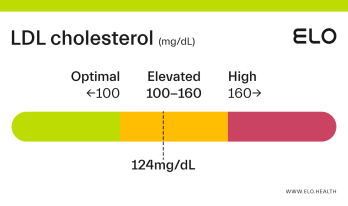
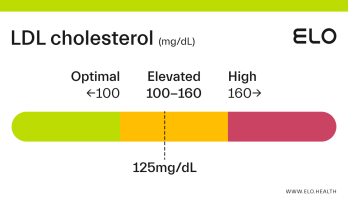
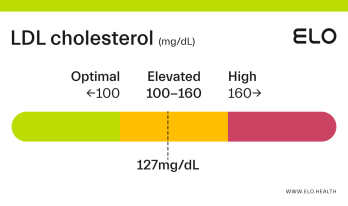
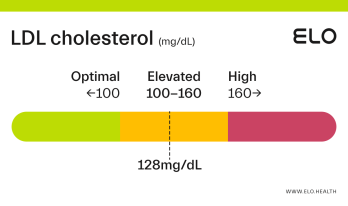
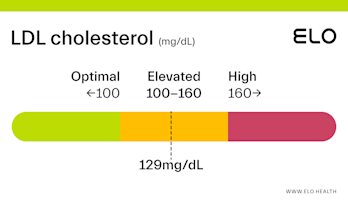
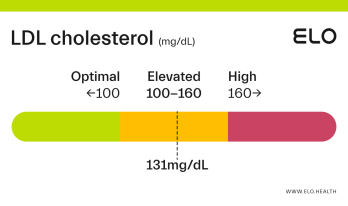
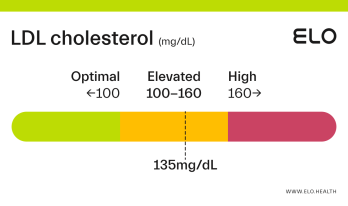
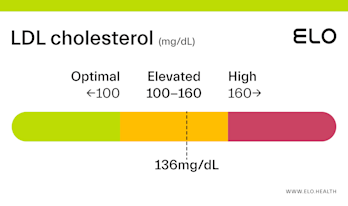
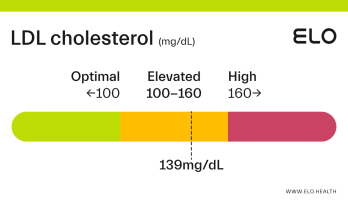
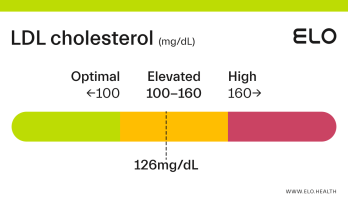
LDL Cholesterol: 126 mg/dL
What does an LDL level of 126 mean? Are there any symptoms associated with this LDL level?
A LDL level of 126 mg/dL is considered elevated. Although cholesterol has several important functions in the body, elevated LDL cholesterol may put you at greater risk for heart disease.
Elevated LDL cholesterol doesn’t have symptoms, which is why it’s important to know your level. Lowering your LDL cholesterol will reduce your risk of developing heart disease and other health issues. If you already have heart disease, lowering your cholesterol can reduce your odds of serious complications, like a heart attack or stroke.
Factors that could contribute to an LDL level of 126:
Diet: Eating a diet that is high in saturated fats, trans fats, added sugar, and low in fiber can cause LDL cholesterol to rise.
Weight. Being overweight also tends to increase cholesterol levels, including LDL cholesterol.
Physical inactivity. Not being physically active can increase LDL (bad) cholesterol and lower HDL (good) cholesterol levels.
Smoking. Smoking lowers your HDL (good) cholesterol which can contribute to a higher level of LDL (bad) cholesterol.
Medications: Certain medications can increase cholesterol levels. These include: corticosteroids, beta-blockers, thiazide diuretics, antivirals, retinoids, and growth hormones.
Diseases: Some diseases like chronic kidney disease, diabetes, and HIV/AIDS can elevate total cholesterol and LDL.
Age and Sex: Premenopausal women tend to have lower total and LDL cholesterol levels than men of the same age. However, cholesterol levels tend to increase with age, in both women and men. After the age of menopause, women's LDL (bad) cholesterol levels tend to rise.
Genetics (heredity): High blood cholesterol can run in families. This is because your genes partly determine how much cholesterol your body makes.
Race. Certain races may have an increased risk of high cholesterol. For example, Blacks/African Americans typically have higher HDL and LDL cholesterol levels than Caucasians.
What to do if your LDL level is 126?
Adopting healthier habits and making changes to your diet can help lower your LDL cholesterol level back into a safe range (<100 mg/dL). Here are some things you can do to help lower your LDL:
Fill up on fiber-rich vegetables, fruit, whole grains, and legumes, and aim to get 30-40g of fiber daily.
Limit the amount of refined carbs and added sugars you eat from foods like soda, crackers, candy, baked goods, sweetened yogurt, and ice cream.
Replace unhealthy trans fats (partially hydrogenated oils) and saturated fats with healthy unsaturated fats; reduce saturated fat intake to < 10% total calories.
Eat small, fatty fish such as salmon, sardines, and trout, at least two times a week.
Move more. Aim to get 30-60 minutes of physical activity most days of the week.
Get at least 2g of plant sterols and stanols daily from food and supplements.
Lose excess weight if you are overweight or obese.
Quit smoking if you smoke.
If you have diabetes, achieve and maintain good blood sugar control (HbA1c).
Medications and supplements used to improve LDL results
If diet and lifestyle changes are not enough to lower your LDL cholesterol, medications and supplements can help lower it to a safer level.
Medications
Medications are typically prescribed if diet and lifestyle changes do not lower LDL cholesterol levels enough on their own. Some common cholesterol medications include:
Statins: Statins reduce cholesterol production in your liver. Because they typically need to be taken for life, statins are only prescribed if diet and lifestyle changes aren’t enough [3]. Some common statin drugs include atorvastatin, simvastatin, and rosuvastatin.
Ezetimibe can be helpful for those with familial hypercholesterolemia and/or who have side effects with statins.
Bile acid sequestrants: These drugs block cholesterol-rich bile acid from being absorbed into the bloodstream and can be prescribed in place of or in addition to a statin.
PCSK9 inhibitors: This medicine is injected under your skin every 2 or 4 weeks and may be prescribed with a statin if you are at high risk of heart attack or stroke, or have familial hypercholesterolemia.
Lomitapide: Typically prescribed if you have familial hypercholesterolemia. Lomitapide requires liver enzyme monitoring as it can cause liver damage and is commonly taken with vitamin E.
Supplements
Plant sterols and stanols: Plant sterols and stanols (also called phytosterols) are found in plant cell membranes and are similar in structure to cholesterol in the body. They block dietary cholesterol from being absorbed and can be found in vegetable oils, nuts, legumes, whole grains, fruits, and vegetables. The average daily intake of phytosterols from food (500 mg) is typically not enough to lower cholesterol, however. Studies show consuming 2000 mg (2 g) of plant sterol and stanols daily from diet and supplements is most effective [4]. Plant sterol and stanol supplements are taken before or with meals can help lower total cholesterol in parallel with other recommended diet and lifestyle changes [4].
Beta-glucan: Beta-glucan is a form of soluble fiber that has been shown to help lower cholesterol levels. It’s found naturally in whole grains like barley, oats, rye, and wheat, mushrooms, and seaweed, and is also available as a nutritional supplement. For cholesterol-lowering benefits, consume 3-7 g/day from your diet and/or a supplement.
Psyllium: Another type of soluble fiber made from the husk of psyllium seeds, psyllium is good for digestive health and regularity, and can also be helpful in lowering cholesterol. Psyllium supplements are sold in powder form and can help reduce lipid levels when taken at a dose of 8-12 g/day.
Alpha-lipoic acid: A potent antioxidant made in the body, alpha lipoic acid is also found in foods including carrots, beets, spinach, broccoli, potatoes, and red meat. Research indicates that 600 mg/day of alpha-lipoic acid from your diet and/or a supplement may help lower total cholesterol and LDL (bad) cholesterol [8].
Bergamot extract: Bergamot is a citrus fruit that has long been used for medicinal purposes. Bergamot extract (made from the juice of the fruit) seems to lower cholesterol and triglyceride levels in adults with high cholesterol [9,10]. One study suggests taking bergamot extract daily for a month may be as effective as taking a low dose of the cholesterol-lowering drug called rosuvastatin (Crestor) [10]. A recent research review indicates that 1000 mg/day may be most effective for lowering cholesterol.
Green tea extract: Green tea extract is a natural supplement made from the leaves of the Camellia sinensis plant that has been shown to help lower LDL (bad) and total cholesterol [11]. A daily dose of 400 mg may help lower your cholesterol but check with your doctor first as green tea extract can interact with certain medications, including beta-blockers and blood thinners. In addition, green tea extract may also have a stimulant effect.
Berberine: A compound extracted from a variety of medicinal herbs, some studies suggest berberine can reduce LDL (bad) cholesterol and triglycerides in type 2 diabetics [12]. It may also slightly increase HDL (good) cholesterol [12]. A standard dose of berberine is 900-2000 mg/day (divided into 3-4 doses), taken with or just after a meal.
References
Cholesterol Levels: What You Need to Know. (n.d.). U.S. National Library of Medicine | NIH. Retrieved September 9, 2021, from
https://medlineplus.gov/cholesterollevelswhatyouneedtoknow.html
Carotid Artery Disease. (n.d.). National Heart, Lung, and Blood Institute | NIH. Retrieved September 9, 2021, from
https://www.nhlbi.nih.gov/health-topics/carotid-artery-disease
High cholesterol. (n.d.). NHS Inform. Retrieved September 9, 2021, from
https://www.nhsinform.scot/illnesses-and-conditions/blood-and-lymph/high-cholesterol
Racette, S. B., Lin, X., Lefevre, M., Spearie, C. A., Most, M. M., Ma, L., & Ostlund, R. E., Jr (2010). Dose effects of dietary phytosterols on cholesterol metabolism: a controlled feeding study. The American journal of clinical nutrition, 91(1), 32–38.
https://doi.org/10.3945/ajcn.2009.28070
Cholesterol: Types, Tests, Treatments, Prevention. (2020, July 31). Cleveland Clinic.
https://my.clevelandclinic.org/health/articles/11920-cholesterol-numbers-what-do-they-mean
Blood Cholesterol | NHLBI, NIH. (2021, January 4). National Institutes of Health.
https://www.nhlbi.nih.gov/health-topics/blood-cholesterol
LDL: The “Bad” Cholesterol. (n.d.). National Institutes of Health. Retrieved September 22, 2021, from
https://medlineplus.gov/ldlthebadcholesterol.html
Mousavi, S. M., Shab-Bidar, S., Kord-Varkaneh, H., Khorshidi, M., & Djafarian, K. (2019). Effect of alpha-lipoic acid supplementation on lipid profile: A systematic review and meta-analysis of controlled clinical trials. Nutrition (Burbank, Los Angeles County, Calif.), 59, 121–130.
https://doi.org/10.1016/j.nut.2018.08.004
Cai, Y., Xing, G., Shen, T., Zhang, S., Rao, J., & Shi, R. (2017). Effects of 12-week supplementation of Citrus bergamia extracts-based formulation CitriCholess on cholesterol and body weight in older adults with dyslipidemia: a randomized, double-blind, placebo-controlled trial. Lipids in health and disease, 16(1), 251.
https://doi.org/10.1186/s12944-017-0640-1
Gliozzi, M., Walker, R., Muscoli, S., Vitale, C., Gratteri, S., Carresi, C., Musolino, V., Russo, V., Janda, E., Ragusa, S., Aloe, A., Palma, E., Muscoli, C., Romeo, F., & Mollace, V. (2013). Bergamot polyphenolic fraction enhances rosuvastatin-induced effect on LDL-cholesterol, LOX-1 expression and protein kinase B phosphorylation in patients with hyperlipidemia. International journal of cardiology, 170(2), 140–145.
https://doi.org/10.1016/j.ijcard.2013.08.125
Xu, R., Yang, K., Li, S. et al. Effect of green tea consumption on blood lipids: a systematic review and meta-analysis of randomized controlled trials. Nutr J 19, 48 (2020).
https://doi.org/10.1186/s12937-020-00557-5
Berberine, Examine. (2021, May 5). Examine.com.
https://examine.com/supplements/berberine/#